Why Patient Preference Matters in Foot Wound Care
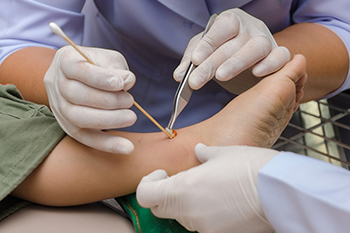
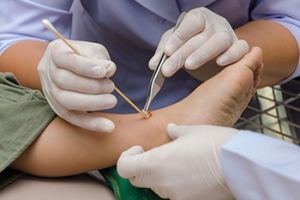
Foot wounds often require specialized attention, but clinical expertise alone is not always enough. The choices patients make about their care matter. From the type of dressings used to how often visits are scheduled, each decision can affect comfort, confidence, and healing. When patients are involved in the planning of their treatment, they are more likely to follow through with care and speak up about concerns. This creates a stronger partnership with the provider and often leads to better outcomes. Respecting personal routines, cultural beliefs, and lifestyle needs helps tailor care that fits into daily life rather than disrupting it. Listening to patient preferences is not just courteous. It is a critical step in treating wounds that are often slow to heal. To create a care plan that truly works, it is suggested that you schedule a visit with a podiatrist who understands the importance of patient input at every stage.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Peter Siroka, DPM from Connecticut. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Stamford, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Categories of Ingrown Toenails

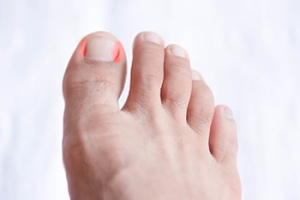
Ingrown toenails are typically classified based on severity and depth of nail penetration into the surrounding skin. A mild ingrown toenail involves redness, swelling, and slight tenderness where the nail edge presses against the skin. A moderate ingrown toenail may cause increased pain, drainage, and signs of infection as the nail begins to pierce the skin. A severe ingrown toenail often includes significant inflammation, pus, overgrowth of tissue, and difficulty walking due to intense discomfort. Chronic cases may result in repeated infections or thickened skin. Each stage may require a different approach to care, from at-home soaking and nail trimming to professional treatment such as partial nail removal. If you are experiencing persistent or painful symptoms, it is suggested that you see a podiatrist for a diagnosis and treatment to prevent further complications and restore comfort.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Peter Siroka, DPM of Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in Stamford, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.
Get Professional Care for a Broken Foot or Ankle
Managing Heel Pad Syndrome
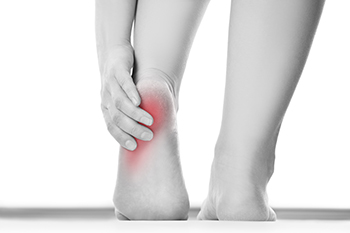
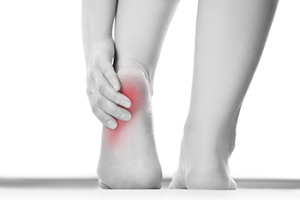
Heel pad syndrome, also known as fat pad atrophy, occurs when the thick layer of fatty tissue beneath the heel thins out, reducing its ability to absorb shock. This can lead to deep, aching heel pain that worsens with prolonged standing or walking. Common causes of heel pad syndrome include age-related degeneration, obesity, repetitive impact activities, wearing improper footwear, and prior heel injuries. People who walk barefoot on hard surfaces may place additional stress on the heel, increasing the risk of pain. A podiatrist can evaluate heel pad function and recommend appropriate treatment to relieve pressure on the heel. Supportive orthotics and well-cushioned footwear can help reduce discomfort during daily activities. In addition, specific exercises, such as calf stretches, heel raises, and ankle range-of-motion movements, are often used to improve foot control and reduce stress on the heel. If you are suffering from heel pain, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and proper treatment.
Many people suffer from bouts of heel pain. For more information, contact Peter Siroka, DPM of Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Stamford, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
What to Look for in Choosing the Right Running Shoes

Selecting the right running shoes is essential for comfort, performance, and injury prevention. Traditional running shoes are designed for roads and tracks, while trail running shoes offer grip and protection on uneven terrain. Shoe selection should be based on gait and arch type. Neutral running shoes work well for those with a balanced gait, while stability shoes support mild overpronation. Motion control shoes are best for significant overpronation. Carbon plated shoes are designed for speed and efficiency in advanced runners. A podiatrist can assess foot structure and gait mechanics to guide proper shoe choice. If you are unsure which running shoes are right for you, it is suggested that you consult a podiatrist for expert advice and personalized recommendations.
If you are a runner, wearing the right running shoe is essential. For more information, contact Peter Siroka, DPM from Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact our office located in Stamford, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Differences between Walking and Running Shoes
Both running and walking are great exercises, but should a person wear the same shoes for both activities? The answer is no, because there is a difference between the way a person’s feet hit the ground when they are walking and when they are running. Therefore, the shoes for each activity are designed differently. Before you begin any exercise program it is always recommended that you speak with your doctor or podiatrist.
Walking is a low impact exercise that is often recommended by doctors to their patients. While walking is a simple activity, it still requires some degree of preparation. If you think about walking and how your feet strike the ground as you move, you will notice that your heel hits the ground first before your foot continues to roll forward and your next step begins. Because of this rolling motion, walking shoes are designed to be more flexible than running shoes. This flexibility helps the walker push off with each step taken.
Because the heel hits the ground first when you walk, walking shoes are designed to absorb most of the shock. Walking shoes should therefore have a beveled or angled heel. The angle of the heel helps absorb the shock and reduces pressure from the ankles. This is especially important for speed walkers, as their feet will hit the ground twice as often as the normal walker.
When people decide to run as a hobby or for their health, they must first realize that running is a high impact exercise. If not done with the proper equipment, running may cause damage to the feet and legs. Running shoes are designed to be more lightweight and to have thicker soles. The thicker soles act as shock absorbers for the rest of the body. Walking shoes often do not have the proper arch support that running shoes do.
A proper fitting shoe can make or break a runner or a walker. If the shoes are too big, their feet will slide back and forth inside the shoe and cause blisters. Whether you will be running or walking, the right equipment can make all of the difference in the world.
Symptoms and Causes of Rheumatoid Arthritis in the Feet
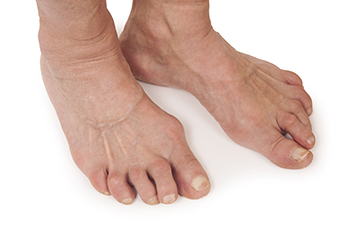
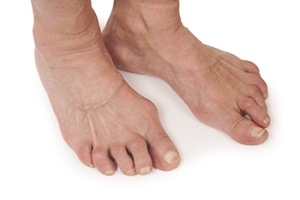
Rheumatoid arthritis, or RA, is an autoimmune condition that often affects the joints in the feet, leading to pain and inflammation. In the feet, symptoms may include swelling, stiffness, and tenderness, particularly in the toes and the balls of the feet. Some individuals may notice warmth or redness around the joints, along with difficulty walking or wearing shoes comfortably. As the condition progresses, joint deformities and reduced mobility may develop. The exact cause of rheumatoid arthritis is not fully understood, but it involves the immune system mistakenly attacking the lining of the joints. Genetic factors, environmental triggers, and hormonal changes may all play a role. Early diagnosis and proper management are important to help reduce pain, preserve joint function, and maintain quality of life for individuals affected by this chronic condition. If you have symptoms of RA and your feet are affected, it is suggested that you are under the care of a podiatrist who can help you to manage this condition.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Peter Siroka, DPM of Connecticut. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Stamford, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.